Conditions
Varicose Veins
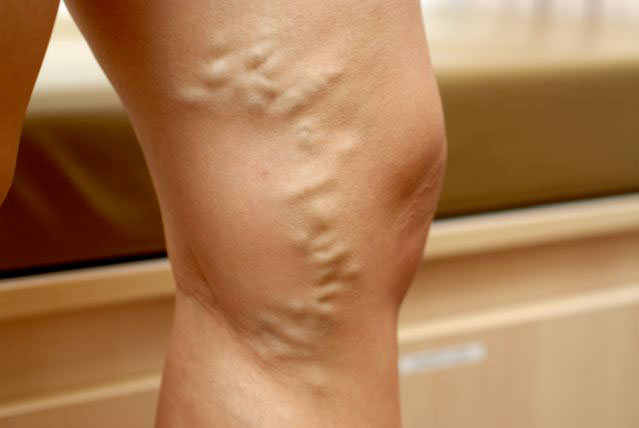
Varicose veins are unsightly stretched veins that protrude through the skin, particularly in the legs. They can occur anywhere from the groin to the feet, but commonly present with bulging in the calf.
Veins are the tubes that carry blood from the body back to the heart. In the legs these tubes have to carry blood upwards against gravity, and so veins contain unidirectional valves to keep the blood flowing upwards. Varicose veins develop when one or more of these valves gives way (often in the groin or behind the knee), and blood starts to flow back down the leg. This increased back pressure on the veins and their branches eventually causes many of them to stretch, lengthen and bulge out, a condition we call varicose veins.
Varicose veins are rarely painful, but may cause increasing discomfort as they enlarge. Frequently the legs will ache, particularly after standing, in hot weather or before a woman's periods. As they progress, itchiness, increased cramping and swelling of the ankles may ensue. Eventually, broken veins (thread veins, spider veins) develop. Skin colour may darken - particularly around the ankle - and in advanced cases complications such as phlebitis, thrombosis or ulceration can occur.
Varicose veins may rarely be congenital (developing from or soon after birth) but more often develop gradually through life. Heredity is the single most important factor in most cases, although pregnancy plays an important part for women who develop varicose veins. They may also develop after trauma or deep vein thrombosis. As with thread veins they occur more frequently in women, and tend to get worse with age.
Varicose veins can be treated at any stage and at any age, provided the appropriate assessments have been performed beforehand.
Consultation and clinical examination is therefore usually followed by Ultrasound Duplex Colour Scanning of the veins. This painless procedure objectively assesses the circulation in the legs and will pinpoint damaged or leaky valves, any blockages or sites of thrombosis.
Treatment can then be targeted to restore the state of the legs to normal, using the most appropriate techniques.
The 3 main aims when treating varicose veins are:
- To treat the underlying cause - usually a leak from one or more valves, commonly in the groin or knee. These leaky valves often end up damaging and making redundant a superficial vein such as the internal or external saphenous vein. Treatment usually requires either keyhole endovenous therapy such as radio frequency (VNUS) or laser ablation. Rarely open surgery may be required in complex cases.
- To remove those lumpy or bulgy varicose veins which have been stretched and elongated. This often requires micro surgery, but in certain conditions may now be treated with Foam Sclerotherapy.
- To obliterate any associated thread or spider veins. These never require surgery, and are frequently treated by micro-injection sclerotherapy (microsclerotherapy) although other techniques, such as laser therapy may also be useful.
Leaky valves usually lead to damage in their associated vein, usually the internal or external saphenous vein, which then requires treatment. This treatment is usually performed using endovenous keyhole techniques, either radio frequency or laser ablation. The damaged vein responsible for the development of superficial varicose veins will have been identified by a Colour Duplex scan and your venous surgeon will advise you on whether they will require endovenous treatment. Endovenous therapy involves sealing off the responsible vein and its leaky valves from within the vein under ultrasound control. There are no incisions or sutures, and treatment is usually performed as a day case. Rarely open surgery may be required in complex situations. Your venous surgeon should be able to advise you on the treatment best suited to you and to your veins.
The main aim of management is to remove these unsightly veins and restore the leg to its normal appearance. In minor cases, this may be a primarily cosmetic procedure, but varicose veins can eventually lead to local damage from pressure or stasis, and in extreme cases to phlebitis (clotting in the varicose vein, associated with a painful, reddened area of surrounding skin). Consequently, most surgeons recommend removal of any varicose veins at the same time as treating the underlying cause. Treatment takes place in one sitting and does not require multiple attendances.
A safe, tested cosmetic procedure for the removal of superficial varicose veins is by Multiple Cosmetic Phlebectomies. This procedure removes the vein via tiny punctures in the skin placed over the vein, which is then removed using a keyhole technique. It requires no suturing, and may be performed under local anaesthetic (if a few veins are present) or sedation (if many veins require removal).
Previously, attempts at sclerotherapy of varicose veins were hampered by a failure to eradicate the veins, the development of staining which could last for years, or in severe cases the development of an ulcer in the skin.
The advent of Foam Sclerotherapy has reduced these problems, and offers an attractive alternative to surgery in some cases. The technique allows greater volumes of chemical to be used without increasing the overall dosage. It is particularly useful in congenital venous conditions, but should not be confused with microsclerotherapy.
Varicose veins are a common problem comprising unsightly stretched veins that protrude through the skin of the legs. A minority of veins if left untreated may lead to problems ranging from aching in the leg and swollen ankles to more serious problems such as phlebitis, thrombosis and ulceration.
Successful management of varicose veins includes thorough examination, relevant investigation which often includes colour duplex ultrasound scanning and appropriate treatment which may often involve some form of keyhole endovenous treatment or foam.
This depends on which stage your veins are at and whether there is any significant damage to the underlying valves. Extension of varicose veins is slow in most people and complications, if they occur, often only present many years after the onset of varicosities. Nevertheless varicose veins will not disappear of their own accord and will gradually worsen with the passage of time. We cannot beat gravity!
No. For the reasons given above the progression of varicose veins in many people is likely to be slow and there are other methods of controlling varicose veins that do not involve surgery. If however there is significant damage to the underlying valves, curing the problem may involve some form of keyhole endovenous treatment such as radio frequency ablation (VNUS). There are a variety of procedures available for the treatment of varicosities, which you should discuss with your venous surgeon.
Strictly speaking no, since most forms of treatment aim at obliterating the varicose vein and dealing with the underlying cause. If this is done correctly, the chances of recurrences are small. Nevertheless, there are some situations such as further pregnancies which may lead to the development of further varicosities in the future. Your venous surgeon will discuss the likelihood of further recurrences with you prior to embarking on any treatment.
Most patients have surgery either as a day case or with a single overnight
stay. All
patients are walking normally the day after surgery and approximately 50%
will be
back at work within a week.
A planned assessment for returning to work is made prior to surgery, and
depends
partly on the work environment (standing, sitting etc), general fitness and
your
usual exercise regime.